Wisconsin
Minnesota rushes to add new hospital beds for COVID-19 surge
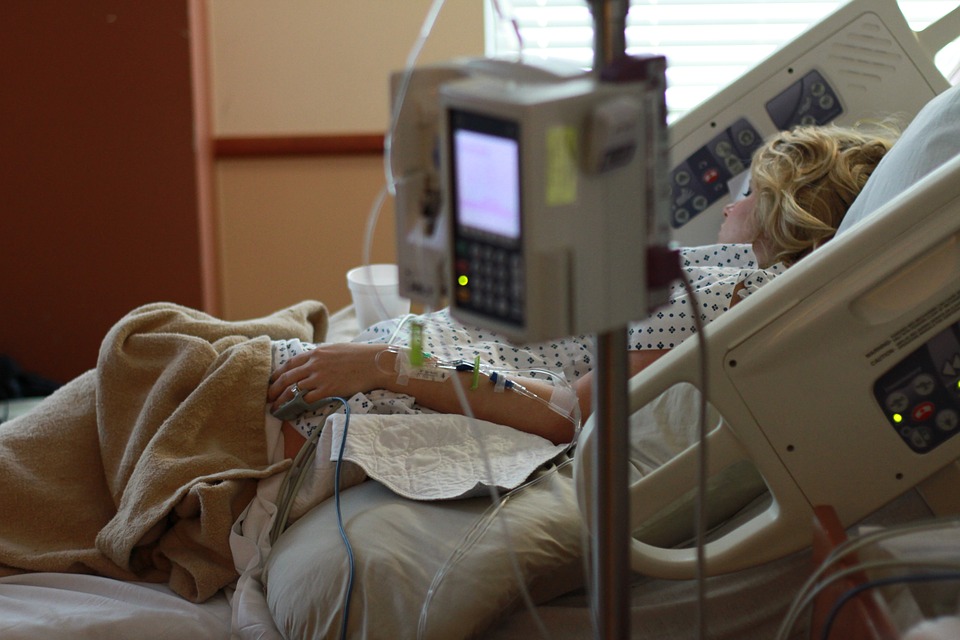
MINNEAPOLIS (AP) — Officials were scrambling Tuesday to set up 2,750 more hospital beds across Minnesota to handle the anticipated surge in COVID-19 cases in the coming weeks.
It’s part of Gov. Tim Walz’s promise to Minnesotans not to waste the time he’s trying to buy with his stay-at-home order to allow the state’s health care system to gear up as the number of cases in Minnesota builds toward a peak in hospitalizations expected between mid-May and mid-June, according to the state’s rough modeling.
Adding to the urgency, the Minnesota Department of Health reported two new deaths Tuesday, raising the state’s total to 12. The state had had 629 confirmed cases as of Tuesday, up 53 from Monday. Fifty-six people were hospitalized, with 26 in intensive care.
The number of occupied intensive care beds is a critical marker. The state currently has just over 260 adult ICU beds available, and Walz has stressed that the goal of his stay-at-home order was to prevent the disease from overwhelming the ability of hospitals to treat the sickest patients.
A team has been identifying potential alternate care sites statewide that could be quickly converted into temporary hospitals for noncritical patients, Joe Kelly, the state’s emergency management director, told reporters during the governor’s conference call with reporters Tuesday.
The immediate goal is to identify space for 2,750 beds, including 1,000 in the Twin Cities area and 1,750 in greater Minnesota, on top of the additional capacity that hospitals are already developing. Minnesota hospitals already had more than 2,400 beds available as of Tuesday, so the new beds would boost capacity for new patients to more than 5,000.
“To be clear, we are not going to immediately build out all these identified spaces and put stuff in them,” he said. “We will convert facilities for this use where and when we need to.”
Once sites are selected and plans are finalized, he said, the state will work with the Army Corps of Engineers to line up contractors. The goal will be to have a facility operational within 48 to 72 hours of deciding to move forward, he said.
“I hope that we never need any of the alternate care sites we’re working on, much less all of them at the same time,” Kelly said.
Kelly has said very little about which sites might be under consideration. He confirmed Monday that the team had evaluated the closed Prairie Correctional Facility in Appleton in western Minnesota.
The M Health Fairview system in the Twin Cities has already remade Bethesda Hospital in St. Paul into a specialized center for COVID-19 patients, expanding it from 50 beds to 90, including 35 ICU beds. Bethesda accepted its first coronavirus patients last Thursday.
At Abbott Northwestern Hospital in Minneapolis, the Allina Health system expects to make 100 more rooms available to COVID-19 patients, including 63 rooms that have already been modified to control air flow.
The Mayo Clinic in Rochester said it was looking at non-traditional areas for additional bed space and working to establish a separate location to triage patients who aren’t critically ill, so it can save emergency department space for the sickest patients.







